CPT add-on codes are one of the first special code types that beginner coders encounter in the CPT codebook. They look like regular CPT codes but come with a very important rule: they can never be reported alone. Understanding CPT add-on codes — how to identify them, when to use them, and what rules apply — is tested on the CPC exam and comes up regularly in real-world coding.
What is an CPT Add-On Code?
An add-on code is a CPT code that describes a service that is always performed in addition to a primary procedure — never by itself. CPT Add-on codes are marked with a plus sign (+) in the CPT codebook, making them easy to identify visually. They represent additional work, additional units of service, or additional complexity that goes beyond the primary procedure.
CPT Add-on codes were created because some procedures are commonly performed in multiples or have optional additional components that not every patient receives. Instead of creating entirely separate codes for every variation, the AMA uses CPT add-on codes to capture the additional service efficiently.
How to Identify CPT Add-On Codes
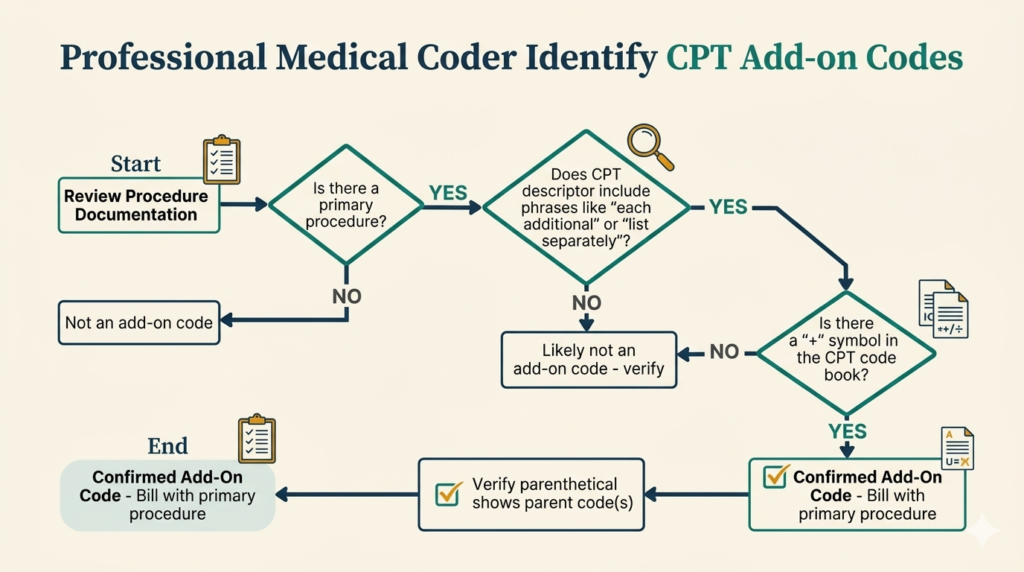
There are three ways to identify add-on codes in the CPT codebook:
- The + symbol appears before the code number in the main section of the codebook
- The code description often includes phrases like “each additional,” “list separately in addition to primary procedure,” or “use in conjunction with”
- Appendix D in the CPT codebook lists a complete summary of all CPT add-on codes
Common Examples of CPT Add-On Codes
| Add-On Code | Description | Primary Code(s) |
|---|---|---|
| +11001 | Debridement of additional 20 sq cm or part thereof (each additional) | 11000 |
| +11008 | Removal of prosthetic material or mesh, abdominal wall for infection (list separately) | 10004–49999 |
| +15301 | Autograft, skin — each additional 100 sq cm | 15300 |
| +99292 | Critical care, each additional 30 minutes | 99291 |
| +99354 | Prolonged service, each additional 30 minutes (outpatient) | E&M codes |
| +01953 | Anesthesia for burn excision/debridement, each additional 9% of body surface | 01952 |
Rules for Add-On Codes
Rule 1 — Never Report Alone
This is the fundamental rule. An add-on code without its primary procedure code on the same claim will be denied by the payer. Always ensure the primary code is listed first on the claim.
Rule 2 — Exempt from Modifier -51
Modifier -51 is used when multiple procedures are performed at the same session — it signals that a procedure is secondary and should be reimbursed at a reduced rate. Add-on codes are automatically exempt from modifier -51 because they are already priced to reflect their supplemental nature. Never append modifier -51 to an add-on code.
Rule 3 — Modifier -51 Exempt Codes Are Different
Do not confuse CPT add-on codes with modifier-51-exempt codes. Modifier-51-exempt codes (marked with ⊘ in the CPT book) are not CPT add-on codes — they are standalone codes that simply do not receive the multiple procedure reduction. Add-on codes are a separate, distinct category.
Rule 4 — Report as Many Units as Needed
Some add-on codes are reported multiple times on the same claim to represent the number of additional increments performed. For example, if a critical care patient required 99291 (first 30–74 minutes) plus three additional 30-minute periods, you would report 99292 three times (or with 3 units).

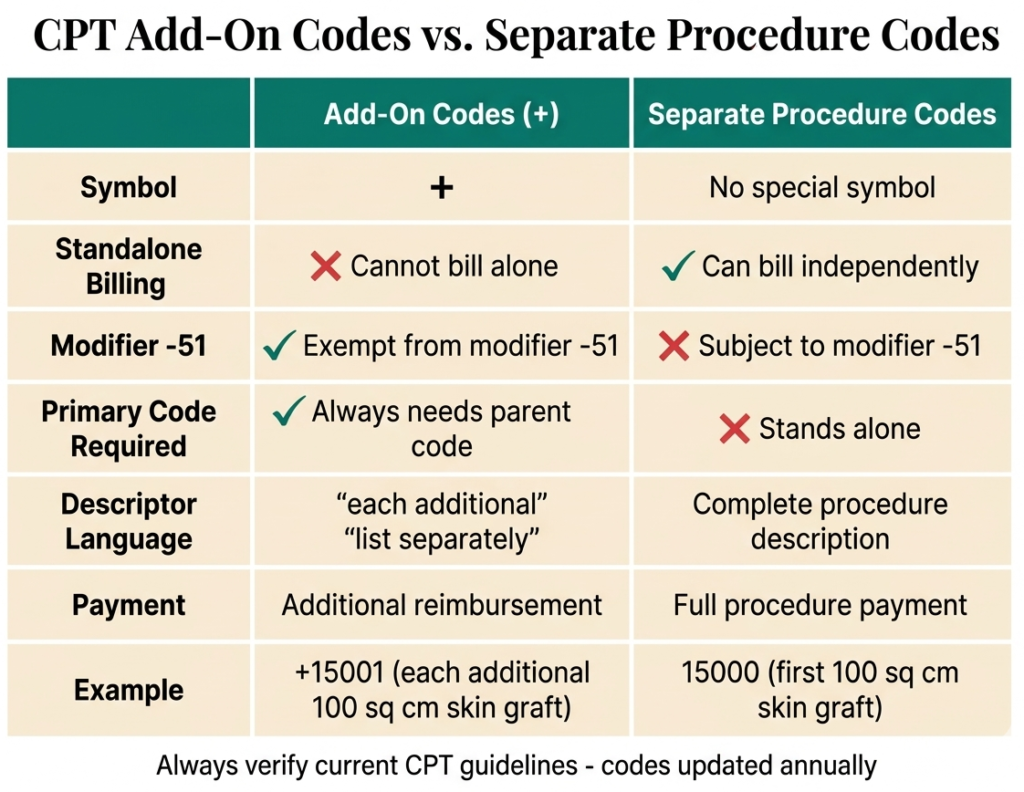
CPT add-On Codes vs Separate Procedures
Add-on codes are sometimes confused with codes marked “separate procedure” in the AMA CPT codebook. These are completely different concepts:
- Add-on codes (+): Always reported with a primary code. Represent additional units or components of care. Never standalone.
- Separate procedure codes: Can be reported alone when performed independently, but are bundled and not separately reported when they are an integral part of a larger procedure.