Bundled codes are one of the most important compliance concepts in medical coding. When two procedures are bundled together, it means one code already includes the work described by another — and billing them separately is considered improper. The National Correct Coding Initiative (NCCI) is the system that enforces these bundled code rules for Medicare and most other payers. Understanding NCCI edits and bundled codes is essential for the CPC exam and for preventing billing errors in real-world coding.
What Are Bundled Codes in Medical Coding?
When a CPT code is said to be bundled into another, it means the work, supplies, and effort described by the smaller code are considered already included in the payment for the larger code. Billing both codes separately would result in double payment for the same service — which is a compliance violation.
Think of it like ordering a combo meal at a restaurant. If you order a burger combo that includes fries and a drink, you cannot also charge separately for the fries and the drink. The fries are bundled into the combo. Medical coding works the same way — certain services are considered part of a larger procedure and cannot be billed separately.
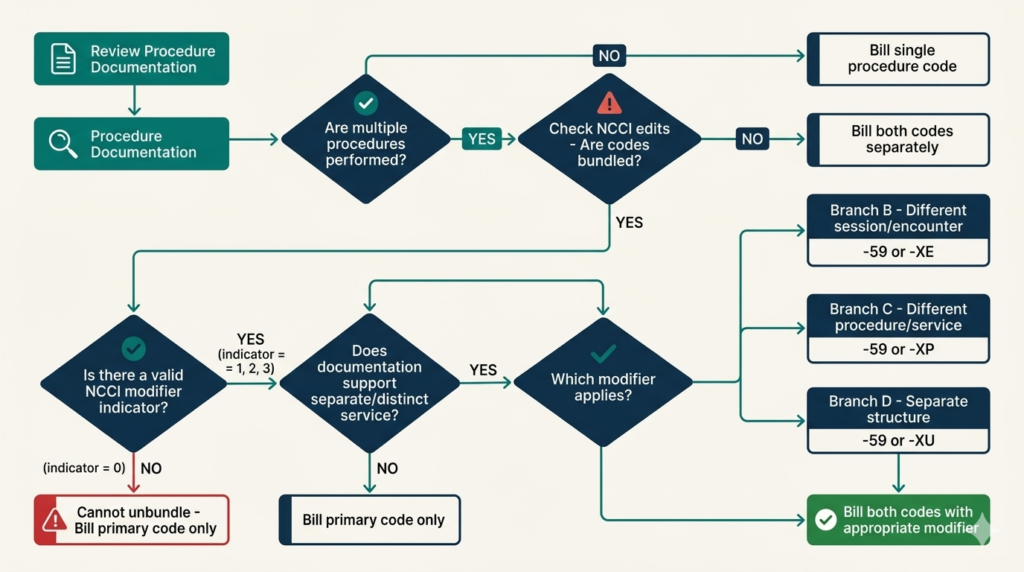
Understanding NCCI Edits & Bundled Codes
The National Correct Coding Initiative (NCCI) was developed by CMS — the Centers for Medicare and Medicaid Services — to promote correct coding and prevent improper payments. NCCI edits are pairs of CPT codes that should not be billed together because one is considered a component of the other.
There are two types of NCCI edits:
- Procedure-to-Procedure (PTP) Edits: These identify pairs of codes that should not be reported together by the same provider for the same patient on the same date of service. One code is the column 1 (comprehensive) code and the other is the column 2 (component) code. Medicare will only pay for the column 1 code.
- Medically Unlikely Edits (MUEs): These set the maximum number of units of service that a provider can bill for a single CPT code on a single date of service. For example, a patient only has two kidneys — so a code for kidney removal should never be billed for more than 2 units.
Common Examples of Bundled Services
| Bundled Into | Because |
|---|---|
| Surgical approach (incision and closure) | Always included in any surgical procedure code |
| Local anesthesia | Included in the surgical code — cannot bill separately |
| Simple wound closure after excision | Included in excision codes — only complex closure is separate |
| Diagnostic endoscopy with surgical endoscopy | Diagnostic scope is bundled when a therapeutic procedure is performed |
| Catheter insertion with certain procedures | Considered part of surgical approach for some procedures |
| Venipuncture with lab draw | The draw is part of the lab collection |
When Can You Override Bundled Codes? Modifier -59 Rules
Sometimes two procedures that are normally bundled are legitimately performed as distinct, separate services on the same day. In these cases, modifier -59 (Distinct Procedural Service) can be appended to the component code to signal to the payer that the services were truly separate and both should be paid.
Modifier -59 is appropriate when the procedures were performed at a different anatomical site, during a different patient encounter, or involved a different lesion or organ. However, it must be supported by documentation — simply adding -59 without clinical justification is considered improper billing.
The XE, XS, XP, XU Modifiers — NCCI Derivative Modifiers
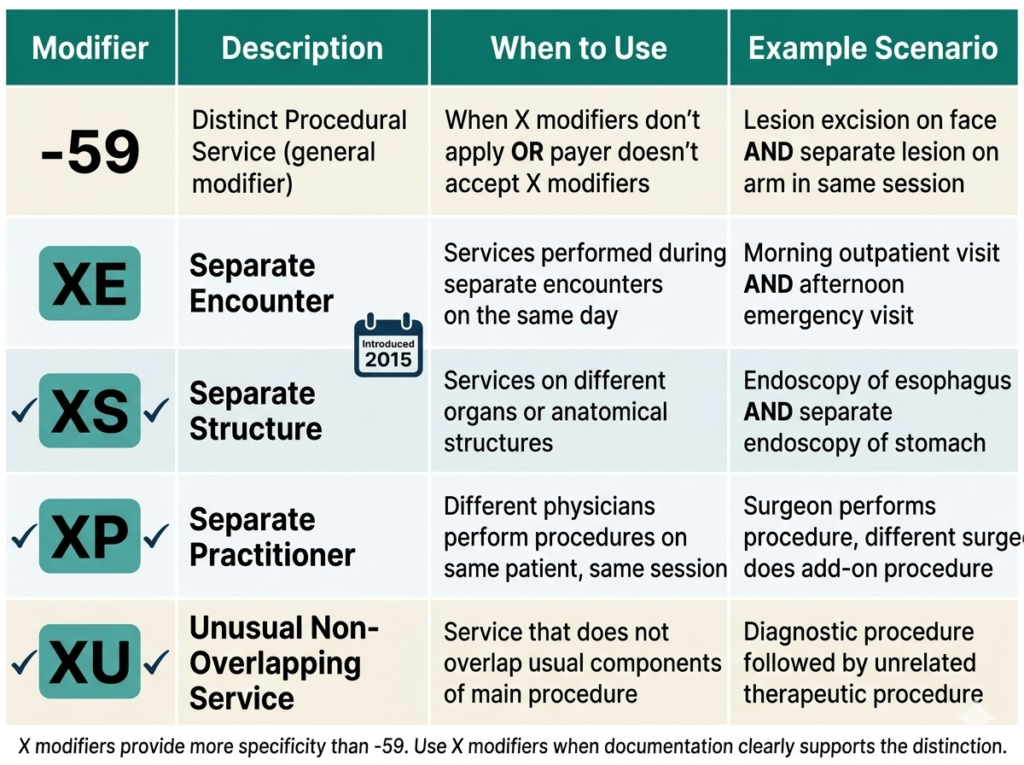
CMS created four more specific modifiers to replace modifier -59 in certain situations. These are called the X modifiers or NCCI derivative modifiers:
- -XE: Separate Encounter — service was provided during a separate encounter on the same day
- -XS: Separate Structure — service was performed on a separate organ or anatomical structure
- -XP: Separate Practitioner — service was provided by a different practitioner
- -XU: Unusual Non-Overlapping Service — service does not overlap with the usual components of the main service
Bundled Codes in Endoscopy: The Surgical Rule Explained
One of the most commonly tested bundling rules on the CPC exam involves endoscopy procedures. The rule states: when a surgical endoscopy is performed, the diagnostic endoscopy is always bundled into the surgical endoscopy code and cannot be billed separately.
For example, if a physician performs a colonoscopy and finds and removes a polyp, you code only the colonoscopy with polypectomy. You do not also code a diagnostic colonoscopy — the diagnostic scope was part of getting to the polyp and is bundled into the therapeutic code.
NCCI Mutually Exclusive Bundled Codes
NCCI also includes mutually exclusive edits — pairs of codes that by definition or medical impossibility cannot reasonably be performed on the same patient on the same day. Unlike procedure-to-procedure edits where one code is a component of another, mutually exclusive codes are simply services that cannot logically both occur. For example, codes for a total and a partial removal of the same organ are mutually exclusive.